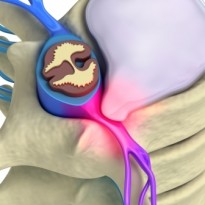
What is a lumbar disc herniation?
A herniated disc is also known as a prolapsed disc but you will probably have heard most people use the term “slipped disc”. This is slightly misleading as your discs physically can’t slip out of place. What has actually happened is that the tough fibers called the “annulus fibrosus” around the outside of the disc have split causing a weakness and allowing the soft material called the “nucleus pulposus” from inside the disc to start bulging out. If you like imagine that your discs are shock absorbers and act like your spines suspension system very much like a car. When you lift a weight the disc compresses, absorbs the weight and disperses it evenly down your spine. Now think of a strong car tyre that’s what the outside fibers of the disc act like and the soft substance inside is similar to the consistency of toothpaste. Any wear, tear or splits in the tyre surface would allow the soft toothpaste to start bulging out. Once the soft substance starts to protrude your body reacts by gathering Inflammation around the bulge. This creates quite severe pain around the disc itself and causes the sudden intense neck pain that sufferer’s first experience.
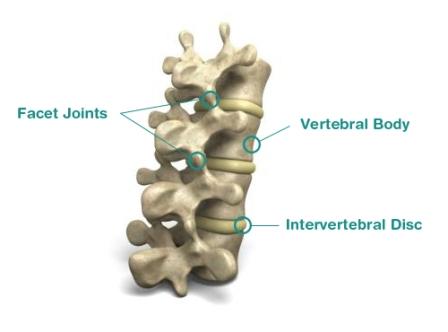
What does a lumbar disc herniation feel like?
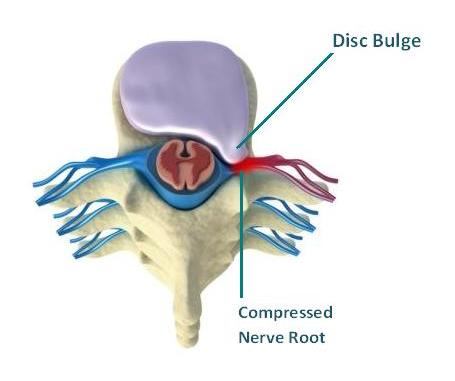
Your lumbar spine surrounds the spinal cord to protect it from damage. Your nerves branch of from the spinal cord and pass out at the level of each disc and then continue to travel down into the leg. The nerve passes very close to the edge of the disc and can be adversely affected by a disc herniation in two ways. Firstly, if the disc bulge is significant enough it will touch and compress the nerve causing pain from the low back to travel down into the leg. Secondly, the leg pain symptoms can be caused by the high levels of inflammation around the disc bulge, irritating the near-by nerve. In many cases the leg pain experienced is overshadowed by severe leg symptoms; as the nerve irritation and pressure can also cause additional symptoms like pins & needles, numbness and weakness down the leg and into the foot.
It is quite possible to have a disc herniation with purely low back pain or no low back pain and only leg symptoms. There have been cases where only minor symptoms or in-fact no symptoms at all have been reported. Rarely, the disc herniation may occur in a slightly different position and put pressure on the spinal cord, this can cause a condition called Cauda Equina Syndrome. Cauda Equina Syndrome is a serious conditionresulting in numbness around the saddle area of the buttocks, a loss of control over bowel and bladder functions or severe increase in frequency and in some cases severe leg weakness and numbness. Cauda Equina Syndrome is considered a surgical emergency and it is advised that upon experiencing these symptoms you should seek immediate medical attention.
The pain is characterized as being an intense ache whilst resting to a sharp, shooting and stabbing pain on movement. The extent of the leg pain and symptoms can lead to sufferers feeling an incredibly heavy leg sensation. Lifting, walking, bending forward and twisting to the side will increase your pain levels. Any sudden coughing and sneezing will be extremely painful.
Why & when does a lumbar disc herniation happen?
There is not one specific reason for the onset of a disc herniation but there are many risk factors that may make you more susceptible. The main factor to consider is disc degeneration. As you get older, the soft nucleus pulposus in the center of the disc starts to dehydrate, retaining less and less water. This decreases the discs ability to act as a shock absorber. The deterioration of the disc in this manner can increase the likelihood of the outer annulus fibrosus layer tearing. Poor posture, previous trauma and a lack of exercise leading to poor core body strength can also leave the spine weakened. These risk factors can lead to early degeneration of the discs especially when combined with obesity and increasing age. Activities which increase the pressure within the disc such as carrying uneven weights, bending in an incorrect manner (back bent and knees straight), holding a prolonged poor seated posture (desk work, driving), direct contact sports and even sneezing can cause the already weakened structure of the disc to give.
A lumbar disc herniation accounts for over 90% of spinal disc herniation cases and occurs most commonly in the lower levels of the low back between L4-L5 vertebrae and L5-S1. Men are twice as likely to be affected as women and it usually develops within the 25-50 year old age range with the highest incidence between 35-45 years.
How long does a lumbar disc herniation take to heal?
The pain levels are normally most severe at the beginning, particularly when the nerve is initially compressed or irritated. Over the first six weeks the herniated bulge should naturally start to shrink and reabsorb back into the disc. Due to this, most cases see a 50% improvement in symptoms with pain levels being dramatically reduced and the additional symptoms like pins and needles, weakness and numbness taking slightly longer to resolve.
What treatments are available for a lumbar disc herniation?
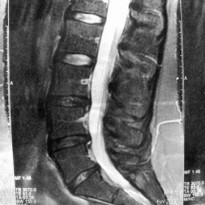
Your GP will be able to diagnose you by both listening to your history and examining you. If symptoms persist longer than six weeks an x-ray or an MRI scan may be advised to confirm diagnosis and assess the size and state of the herniated disc. In these more severe cases surgery may be necessary however this only represents a minority group as only 1 in 10 cases are considered for surgery.
Most cases of lumbar disc herniation will improve without surgical intervention. Others find alternative therapies speed up the recovery process and alleviate the high pain levels. Your GP may advise a short period of rest after the initial onset when pain levels are high, however it is very important that after two or three days you begin moving again to prevent your neck joints from stiffening and your neck muscles from weakening. Your GP may prescribe you with anti-inflammatory medications to reduce the swelling around the bulge and analgesic medication for pain relief. You can help yourself by using ice packs on your low back to control the inflammation levels. Make sure the ice pack is covered to prevent ice burn and restrict the time you apply it to 10-15 minutes with at least 30 minutes intervals. Once you start to recover it is very important that you get rehabilitation exercises to strengthen your low back. This can be done through the relative therapist or trainer. In most cases the low back is left weak after a herniated disc, strengthening your core muscles will ensure you make a full recovery and dramatically decrease future occurrences. It is advisable to seek medical advice from your GP before commencing your rehabilitation exercises.