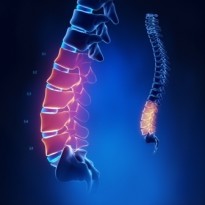
What is thoracic degenerative disc disease?
Thoracic degenerative disc disease known as thoracic DDD is in fact not a disease and medical professionals even debate whether it is in fact a degenerative condition. The misleadingly named diagnosis is used as a term to describe a condition that affects the discs in your spine (not including a disc herniation) and accounts for a lot of neck pain cases. The condition is a weakening of the discs in the spine and normally once DDD is at the stage of diagnosis there are multiple disc levels involved.
Why & when does thoracic degenerative disc disease happen?
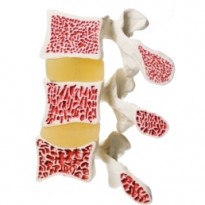
Disc Degeneration occurs naturally with age and most people over 30 will have some form of disc degeneration present within their spine but might not necessarily have any symptoms, whilst others may experience symptoms at an earlier age developing after trauma or repetitive injuries to the back. The discs in your spine are cushioned in between the spinal vertebrae bones. The role of your discs is to act as shock absorbers creating your spines vey own suspension system very much like in a car. When you lift a weight the disc compresses, absorbs the weight and disperses it evenly down your spine. Now think of a strong car tyre that’s what the outside fibers of the disc wall act like and the soft substance inside is similar to the consistency of toothpaste. Injury can cause tears to occur in the tough outer fibers of the disc wall called the “annulus fibrosus” creating the first of the pain levels. Your body is designed to repair some of this daily disc wear, however once healed the torn fibers are replaced by innervated scar tissue which is a lot weaker than the original fibers and also a lot more sensitive.
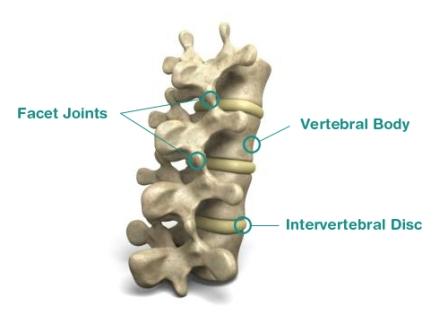
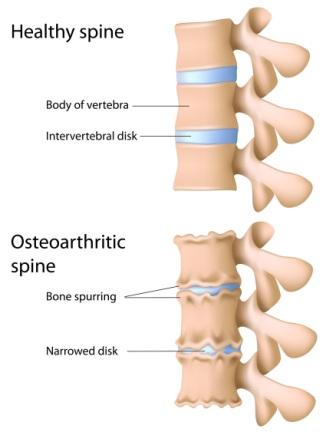
Your back depends on your discs and joints to link the spinal vertebrae not only to allow but also to control the movement of your back. Now consider how much you move use your back on a daily basis and then imagine how much stress these discs must injure over your lifetime. The end result of this is repetitive tears and injury to the disc wall significantly weakening it. This increases the pressure on the soft material inside the disc called the “nucleus pulposus”. As you get older, the soft center of the disc starts to dehydrate, retaining less and less water. This decreases the discs ability to act as a shock absorber. The deterioration of the disc in this manner combined with the weakening of the disc wall causes the inside of the disc to collapse. This significantly decreases the height of the disc space and allows the vertebrae above and below to slide closer together. This also has an impact on the two facet joints either side of the disc causing them to approximate, twist and damage their joint surfaces. The exposed damaged joint surface on the outskirts of the joint and around the rim of the vertebrae react by growing new bone spurs called osteophytes. This is in attempt to compensate and stabilise the now twisted and pressurized joint or disc. These changes to the spine are also seen in thoracic osteoarthritis.
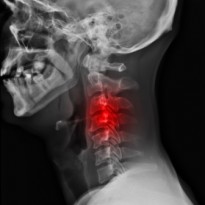
Your thoracic spine surrounds the spinal cord to protect it from damage. Your nerves branch of from the spinal cord and pass out at the level of each disc and then continue to travel around into. The spinal cord and nerve passes very close to the edge of the disc and can be adversely affected by any boney growths that may impinge the nerve or spinal cord. When a nerve is impinged there are additional symptoms like pins & needles, numbness and weakness down the arm and into the hand. When the spinal cord is impinged this leads to spinal stenosis which could cause severe problems in the arms and legs.
What does thoracic degenerative disc disease feel like?
Thoracic DDD is a slow and gradual condition that occurs over many years. The pain levels can be mild from day to day however as the condition worsens the pain levels can be very high. Initially thoracic DDD presents itself as moderate to severe upper back pain and stiffness that comes and goes as the disc is tearing and healing The pain has been described as a sharp pain, an intense dull ache almost like toothache and also like a burning sensation. Due to the fact that DDD normally involves more than one disc then it is more likely to feel like generalized upper back pain rather than a pin point pain location. The inflammation levels from the collapse of the inside of the disc irritate the sensitive newly innervated scar tissue in the disc wall causing an increase in the pain levels. Also at this stage the disc no longer has any cushioning properties and is unable to resist and control movements creating yet more pain.
Gradually as the disc becomes progressively injured and the boney growths develop then the symptoms of pain in the neck may develop into the side pain with the addition of pins and needles and numbness coupled by intense stiffness leading to severe loss of upper back mobility. As a result of the stiffness and secondary to the pain, the muscles surrounding the upper back may start to weaken, and the ligaments may become more lax. This can lead to unstable and more injury prone back. The surrounding muscles and tendons may start to spasm and contract this is a compensatory reaction with the aim to secure and support the joint. The stiffness levels are characterized by stiffness worse first thing in the morning that improves after moving around for half an hour to an hour. Pain levels gradually worsen throughout the day reaching the worst levels in the evening. Rest and lying down provides the most relief as do gentle movements and heat packs over the affected area. Prolonged static postures like sitting and activities like bending and lifting aggravates pain levels. Interestingly in some cases with quite progressed DDD only mild symptoms are experienced.
How will thoracic degenerative disc disease be diagnosed?
Your GP or therapist will be able to diagnose you by both listening to your history and examining you. An X-ray of the affected area is normally recommended to confirm the diagnosis and to evaluate the level and extent of the disc degeneration.
What treatment options are available for thoracic degeneration disc disease?
Treatments for thoracic DDD are usually nonsurgical, however in the occasions where nonsurgical treatments are not affective after two to three months and in cases where the side or leg pain, weakness and numbness limit your daily activities then surgery will be considered. There are many different types of surgery offered for DDD however the most common surgery is spinal fusion to stabilise the affected spine but artificial disc replacements or facetectomy are also used to recover the disc height and joint space. Spinal surgery carries high risks therefor it is only considered on an individual basis if the benefits outweigh the risks.
Unfortunately there is no cure for degenerative disc disease. Instead treatment is normally aimed at reducing pain levels, maintaining mobility and preventing further degeneration. Sufferers normally opt for a combination of treatments, most importantly modifying their lifestyle and avoiding or adapting certain activities to minimise any potential discomfort. It is incredibly important for people who are overweight to factor in weight loss as part of their treatment as it has been shown to radically reduce pain and stiffness levels as the pressure on the discs is reduced. Rest is important through the severe flare ups but it is equally important to start lightly exercising your back as soon as you feel you can. Light exercises provided by your therapist or trainer will not only strengthen your back but also maintain its flexibility and help prevent any further back stiffness. Many sufferers find manual manipulative therapies such as chiropractic, osteopathy and physiotherapy to be helpful in preventing the severe flare ups but also help with the general day to day stiffness and pain levels.
Your GP will most likely prescribe anti-inflammatory painkillers to reduce and control the painful inflammation that occurs with the severe episodes. In more severe cases your GP may use muscle relaxants or even spinal injections to reduce inflammation, pain and relax any muscles spasms. You can help yourself by using either heat or ice. Which one will depend on the individual person some sufferers prefer to use a cold or heat pack. It is advisable to apply them in the evening or after any painful activity like a long day at work or gardening. An ice pack should be covered and applied for 10-15 minutes and left off for 30 minute intervals whereas a heat pack should be left on the affected area for 20-30 minutes. Tens machines are also found to be helpful.