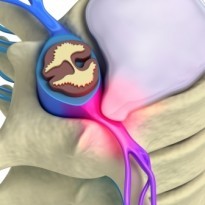
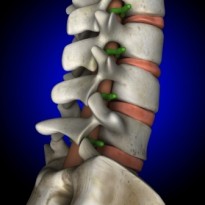
What is lower-crossed syndrome?
Lower-Crossed Syndrome or lower-cross syndrome is the term for a particular pattern of muscular imbalance in the lower body. Lower crossed syndrome is characterized by tightness of the thoraco-lumbar extensors in the lower back, rectus femoris in the back of the thigh and the iliopsoas that passes from the low back to the front of the hip. This pattern of tightness is reflected by weakness of the abdominal muscles in particular the transversus abdominus and the gluteal muscles of the bum.
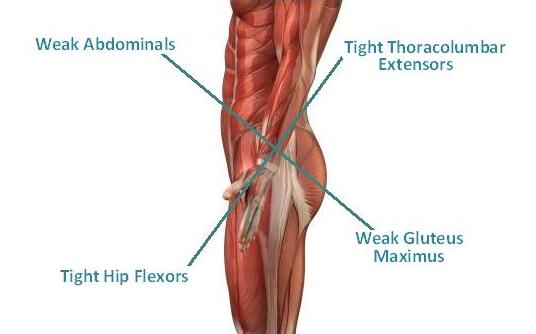
This pattern of imbalance creates joint dysfunction at particular points within the spine. Like the L4-L5, L5-S1 segments and SI joints of the low back and the hip joint. Janda, who first discovered the syndrome, noted that these focal areas are points of stress within the spine.
Layer syndrome named due to the alternating layers of muscular weakness to tightness throughout the postural muscles is a combination of the upper-crossed syndrome and lower-crossed syndrome.
Why and when does lower-crossed syndrome happen?
There are several factors involved in the development of lower-crossed syndrome, one of those is thought to be a previous injury to the joints, ligaments or muscles in the low back, pelvis or hip that doesn’t resolve completely and leaves certain muscles tight and short. This shortening and tightening of the muscles can also occur from repetitive activities or with poor posture, in particular poor core abdominal muscles often leave the lower back and pelvis less supported and more likely to develop muscular imbalances. Once a group of muscles have become tight and short, the relative opposite muscle groups become weakened and as a result the previous mentioned tight muscles tighten further. This starts a negative feedback cycle that if undisturbed accentuates the muscular imbalance.
What does lower-crossed syndrome feel like?
The most common result of lower-crossed syndrome is specific postural changes; however these postural changes can, if left, be a contributing factor to injury development and recurrence. Facet joint strains as well as pelvic and hip dysfunction are all likely conditions that may develop due to the altered muscle balance. The specific postural changes noticed include anterior pelvic tilt where the pelvis overly tilts forward, increased lumbar lordosis (the spinal curve of your low back), lateral lumbar shift, lateral leg rotation (outwards rotation), and knee hyperextension.
The most common result of upper-crossed syndrome is specific postural changes; however these muscular imbalances can, if left, cause the surrounding low back, pelvis and hip joints, ligaments and muscles to loose mobility becoming a contributing factor in the development and recurrence of injuries. Facet joint strains as well as pelvic and hip dysfunction are all likely conditions that may develop due to the altered muscle balance. The resultant increased stress on certain joints can also cause early degenerative joint disease also known as Osteoarthritis.
The postural changes noticed include anterior pelvic tilt where the pelvis overly tilts forward, increased lumbar lordosis which is an increase in the spinal curve of your low back, lateral lumbar shift, lateral leg rotation when your leg rotates out away from the body and knee hyperextension.
How is lower-crossed syndrome diagnosed?
Your therapist will be able to diagnose you by listening to your history, looking at your posture and examining you. Your therapist will look at your posture in detail and may line you side on against a plum line to measure how altered your posture has become. The examination will consist of muscle palpation and stretching to locate the short and tight muscles and muscle testing to determine the weaker muscle groups. Your therapist will also look at the movement of all of the surrounding joints to check for underlying or causative factors. No X-rays or any further investigations are needed to confirm the diagnosis.
What treatments are available for lower-crossed syndrome?
Short term treatment will focus on restoring the mobility of your joints through joint manipulation and relaxing the overly tight muscles with massage. The best types of therapist for this condition are therapists who can treat both joints and muscles, namely Physiotherapists, Chiropractors and Osteopaths. Treatment alone will not be enough to reverse the muscular imbalance therefore your therapist will also prescribe you with exercises. Specifically mobility stretches for the tight muscles in your lower back and thighs with more specific corrective strengthening exercises for the weak gluteal and abdominal muscle groups. In the long term it is important that you maintain a good working posture to avoid recurrence, however sometimes
Once you have recovered it is important to prevent any muscular imbalance from developing again. If the tension has built up from poor posture or weakness then it is extremely important that you look at your office chair and desk layout as well as maintaining your prescribed exercises. Pilates or Yoga are very good at strengthening your core and improving your posture and treatments such as the Alexandra technique are very good at educating your posture. If improving your posture and maintaining the exercises hasn’t been enough to prevent muscular tension from building,then you may find it is helpful to receive regular massage treatments, in these circumstance therapists like Bowen technique, massage therapists and sports therapists are recommended.






.jpg)







.jpg)