What is a pelvic fracture?
A Pelvic fracture is a fracture of any part of the pelvis including the pubis, ischium, and ilium. The pelvis is also known as the pelvic girdle or the pelvic bone; it forms the bony structure that bridges the gap between the spinal vertebrae and the legs. Initially the pelvis starts as three bones (pubis, ischium and ilium) that merge together as you grow into adulthood. Once they have formed the Pelvic structure is made of two symmetrical bones that are connected at the back by the wedge shaped sacrum bone; creating two joints either side called the sacroiliac joints and joined at the front to create the pubic symphysis. The Pelvis is interlaced with many very strong ligaments that add to the durability of the structure. The word pelvic is derived from the Latin word ‘basin’ as the boney structure creates a bowl like cavity that houses most of the digestive and reproductive organs of your body along with main arteries and nerves. Due to the close proximity of these fragile internal structures certain pelvic fractures can cause complications like internal organ damage, nerve damage or internal bleeding there-fore any Pelvic fracture is deemed a medical emergency until known otherwise.
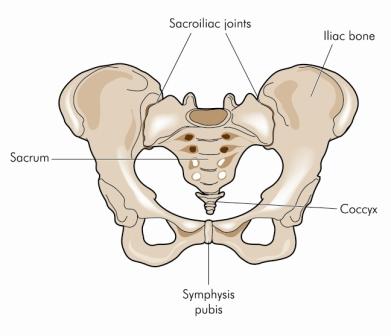
Why & when does a pelvic fracture happen?
Your pelvis is a very durable structure strengthened further by its many interlaced ligaments and surrounding muscles. Due to this most Pelvic fractures are caused by high energy impact injuries such as those sustained from car accidents, crush accidents and falling from a height such as falls whilst cycling or horse riding.
The pelvis is slightly weaker during the growth stages in teenage years as the bone is not as strong. Teenagers who play sports that involve sudden movements may experience a type of fracture called an avulsion fracture. An avulsion fracture happens when there is a sudden contraction of a muscle and the tendon to which it is attached to the bone by pulls and breaks off a small portion of bone. Due to the nature of the injury it is commonly misdiagnosed as a pulled muscle. The pelvis is also weakened in elderly people with osteoporosis. Osteoporosis actually weakens the inner structure of the bone meaning that fractures can occur from less forceful falls including slipping on the stairs, falling whilst getting out of the bath and even just falling from standing.
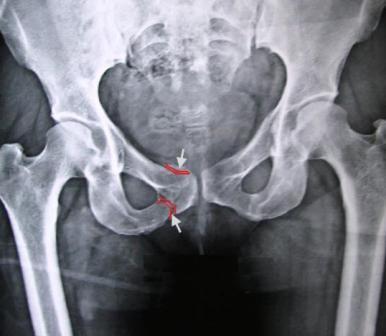
What to do if a pelvic fracture is suspected after trauma?
If you suspect someone has sustained a Pelvic fracture after trauma then you must immediately call for medical help. Most people in high impact accidents sustain other injuries as well as a pelvic fracture making medical attention vital. It is important to make sure the individual is safe and comfortable without having to move the individual as any walking or weight bearing will be very painful. On arrival paramedics will stabilise the pelvis, normally on a stretcher before taking the patient to accident and emergency.
What does a pelvic fracture feel like?
A pelvic fracture causes a very intense immediate sharp pain. The fracture is often accompanied by swelling and bruising and aggravated by most movements this makes weight bearing and walking excruciating. Any movement of the hip muscles may increase pain levels causing many people to adopt a curled up position with their knees and hips bent in a way that doesn’t put any pressure over the pelvis. The intense pain after a break will last for several hours which will be aggravated or prolonged by any treatment options like manipulation or traction. Post-surgery or treatment when the bone starts to heal there will be a dull continuous ache from the swelling and healing process that will last weeks to months. During the healing process the bone is trying to knit together and re-unite this stage can be quite painful and it is very important to rest through this stage to ensure that the bone reconnects properly. The soft tissue surrounding the fracture also starts to form scar tissue to bind everything together allowing the structure to try and restore its original state and function.
How will a pelvic fracture be diagnosed?
Patients will be taken to A&E and a full abdominal and neurological examination will be done to rule out nerve, artery or organ damage. Your doctor will order an X-ray of the pelvis to confirm the diagnosis and identify the location and the extent of the fracture. If your doctor wants to assess the fracture further then a CT scan will be ordered as this will give a more detailed view of the fractured site. A CT scan will also be ordered in cases where damage to the internal structure or nerves is suspected. Occasionally ultrasound will be used to check for bleeding or fluid in the pelvic cavity.
What treatment options are available for a pelvic fracture?
The treatment options and healing times for pelvic fractures varies depending on the severity of the fracture and also on the complications from any additional injuries. Stable fractures such the avulsion fractures and fractures related to osteoporosis are not likely to require surgery. Patients will initially have to rest and avoid weight bearing and will be required to use Crutches or a Zimmer frame whilst recovering. The doctor will most likely prescribe anti-inflammatory medication and painkillers for pain relief and to reduce any swelling. A pelvic fracture can take anything from 8 -12 weeks to heal if not longer. You will be referred through to a physiotherapist who will provide you with exercises to strengthen your pelvic floor, hip and low back muscles to aid the healing process.
In cases of unstable pelvic fractures surgery is almost always necessary. These are the fractures that are a result of high impact car accidents, crush or fall injuries. The Surgery will ensure that the pelvis is stabilised. The type of surgery required will depend on the extent of the fracture. Patients will have restricted mobility for several months after which intense rehabilitation to strengthen the pelvic, low back, hip and leg muscles will be needed. Fluctuating pain levels will be experienced throughout the healing process however most of the discomfort towards the end of the healing process comes from stiffness levels. The rehabilitation exercises as well as massage and some manipulative therapies can aid in recovering your hip and low back flexibility.