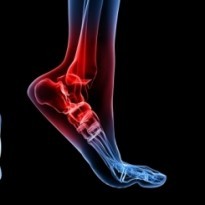
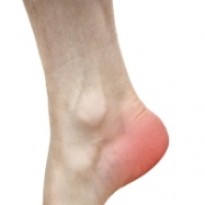
What is flatfoot?
Flatfoot also known as fallen arches or pes planus is a condition in which the medial arch of the foot collapses. The extent of the collapse causes the sole of the foot to come into partial or complete contact with the floor when standing. The foot consists of three arches a transverse, longitudinal and medial arch. The arches are formed by the main bones of the foot mostly the tarsal and metatarsal bones and are reinforced by the surrounding soft tissues including ligaments, tendons, and muscles. The arches are designed to absorb any impact, acting as shock absorbers and distribute body weight evenly and limit the amount of pressure through the joints of the foot. There are various types of flatfoot including adult acquired flatfoot, paediatric flatfoot and flexible flatfoot.
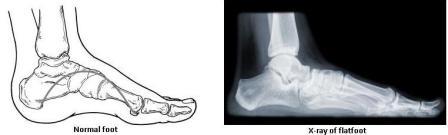
What is paediatric flatfoot?
Paediatric flatfoot is common in both children and adults it is classified as symptomatic or asymptomatic. Symptomatic flatfoot develops symptoms such as pain, tenderness and cramping in the foot. The heel will likely be tilted outwards and the child will struggle with wearing shoes. The child will most likely avoid physical activities. Most children with flatfoot however have no symptoms termed as asymptomatic flatfoot. The condition can be apparent at birth but may not be diagnosed until later in life.
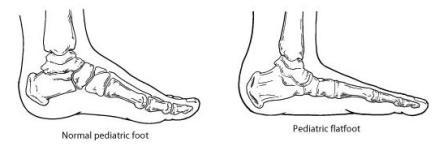
What is flexible flat foot?
Flexible flatfoot is one of the more common types of flatfoot typically beginning in childhood or adolescence and continuing into adulthood. Flexible flatfoot is aptly named due to the fact that with this certain type of flatfoot the arch is collapsed when weight-bearing but returns to normal once there is no pressure through the foot. This type of flat foot will start as a mild deformity that normally occurs in both feet and will progress with time. As the deformity progresses the surrounding tendons and ligaments will stretch and tear causing increased pain and inflammation along the heel and arch. The heel will likely be tilted outwards this change in foot posture will increase pressure upon the knee, hip and low back causing increased likelihood of developing pain and discomfort in these areas.
What is adult acquired flat foot?
Adult acquired flatfoot is also known as posterior tibial tendon dysfunction is the most common type of flatfoot to develop in adults. It is a condition that occurs due to trauma or overuse of the posterior tibial tendon. The injured tendon becomes lax and is no longer able to support and sustain the arch leading to partial or complete collapse. This type of flatfoot will start as a mild deformity that will progress if left untreated. Unlike flexible and paediatric flatfoot, adult acquired flatfoot normally occurs in one foot but can occur in both feet. Symptoms normally occur after physical activity in which the tendon has been stressed such as running, walking or hiking. Symptoms include pain and swelling along the heel and arch and as with other types of flat foot you will notice the heel of the affected foot tilts outwards. Due to the change in foot posture it is highly likely to experience additional ankle and shin pain.
Typical characteristics of flatfoot;
Most types of flatfoot share these characteristics including:
• “Toe drift,” which is where the toes and front portion of the foot starts to drift to the side causing your toes to point outwards.
• The heel will typically tilt toward the outside and the ankle appears to turn in on itself.
• The Achilles tendon will most likely tighten due to the altered foot posture this will cause the heel to lift off the ground earlier when walking and may perpetuate the problem.
• Bunions and hammertoes may start to develop these are a common result of flatfoot.
How is flat foot diagnosed?
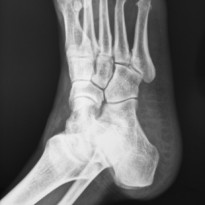
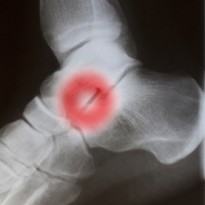
Your GP or podiatrist/chiropodist should be able to diagnose you by listening to your symptom history and thoroughly examining the foot and ankle including the foot posture when sitting, standing and walking. In certain cases the doctor will also examine the hips and knees to rule out additional problems. Your doctor will most likely order an X-ray of the foot to determine the extent of the deformity.
What treatments are available for flatfoot?
The treatment options for flatfoot vary depending on how early the condition is diagnosed. The earlier the condition is diagnosed, the easier it is to treat. Therefore, it is advisable that report to your doctor when you first notice symptoms. Due to the progressive nature of adult acquired flatfoot early treatment is essential and will radically decrease the need for surgical intervention and prevent the early onset of ankle & foot arthritis.
Conservative treatment options for flatfoot include shoe modifications with arch inserts or orthotics to improve and support the arch posture or biomechanics. The doctor will most likely prescribe anti-inflammatory medication and painkillers for pain relief and to reduce any swelling there is also the option of corticosteroid injections to reduce persistent inflammation and pain. Occasionally a cast will be used to immobilise the foot and allow the foot to heal in a non-weight-bearing environment. Your doctor may also refer you to a podiatrist/chiropodist or physiotherapist who may use ultrasound or manual therapy to reduce pain levels.For children with asymptomatic paediatric flatfoot treatment is often not needed. Doctors may elect to prescribe orthotics designed to support the arch and will monitor the deformity periodically to ensure that it isn’t progressing.
Doctors will normally only recommend surgical intervention for flatfoot in more severe, progressed cases or when conservative treatment fails. You will be referred to a specialist ankle and foot orthopaedic surgeon who will recommend the type of surgery based on your health, activity level and the severity and extent of your condition. The recovery and results you see after surgery will vary, depending on the type of procedure performed.