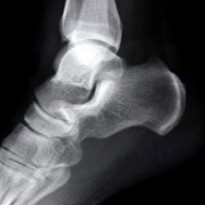
What is tarsal coalition?
Tarsal coalition is a medical term used when the two or more of tarsal bones at the back of the foot are fused. Tarsal coalition is a congenital condition meaning it has occurred from Birth. The Foot itself is made of 3 sections of different bones. The bones at the back of the foot under the ankle joint are known as the Tarsal bones which include the calcaneus (which forms your heel), the talus (which forms part of the ankle), Navicular, Cuboid, and the lateral, intermediate and medial cuneiforms. The next section is the mid foot consisting of the 5 long metatarsal bones, numbered in the sense that your big toe is 1st and your little toe is your 5th. The metatarsals connect at the back to the cuneiforms, navicular and cuboid bones and at the front to the toes. The toes are the last section consisting of 5 bones called phalanges which like the fingers are individually divided into three bones (distal, middle and proximal) the big toe is referred to as the hallux and has only two bones. The tarsal bones play an important role in the biomechanics of the foot. Not only do they form a portion of the ankle joint but they also contribute to and support the structure of the foot arch thus affecting balance and supporting weight-bearing stances.
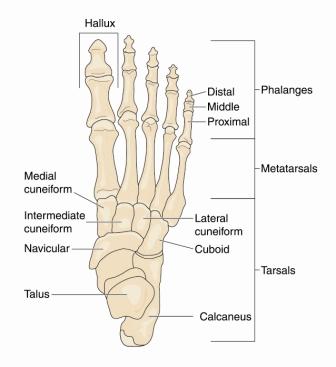
Why & when does tarsal coalition happen?
Tarsal coalition is a relatively uncommon condition affecting only a small proportion of the population. The reason for this congenital condition is unknown but it is thought to be a birth defect meaning that during development when the tarsals which are meant to separate an error occurs and two or more of the bones are left conjoined. The condition is linked genetically and can normally also be found in the parents or grandparents. Problems and injuries associated with tarsal coalition normally start to manifest in adolescence in particular from increased athletics activity.
What does tarsal coalition feel like?
In many cases tarsal coalition is a silent condition meaning it doesn’t cause and symptoms of pain or discomfort however this is not always the case. The coalition of the tarsals itself does not cause pain but the altered way in which the foot works due to the coalition can create problems. The tarsals are designed to distribute your weight through the foot and to support the movement of the foot when walking and running. To begin with the tarsals are mostly very soft bones meaning that in infancy they can bend against pressures but as the skeleton starts to mature in adolescence they ossify and harden. It is at this point where symptoms may begin. Once the coalition has hardened the foot may no longer have as much flexibility and its ability to distribute weight and act as a shock absorber will decrease. Due to these biomechanical changes and resultant stiffness in the foot there will be increased pressure on the surrounding structures including the ligaments and muscles of the foot and lower limb. The stresses placed upon these structures creates allot of the discomfort felt and can often result in recurrent ankle sprains and cases of tendonitis. The pain levels will normally be increased by any weight-bearing activities such as running, dancing and jumping.
How will tarsal coalition be diagnosed?
Your GP or therapist will be able to diagnose you by both listening to your history and examining you. A full examination will be done to rule out any additional injuries or complications. Your doctor will most likely order an X-ray of the foot to confirm the diagnosis and identify which tarsals are conjoined. Occasionally if the tarsal coalition is not fully visible on an X-ray then an MRI or a CT scan will be ordered as this will give a more detailed view. Doctors may also use an MRI scan or further tests to assess where the pain felt is coming from whether it be an injury to the leg muscles, ligaments or joint capsule. The presence of tarsal coalition in one foot may prompt the Doctor to X-ray the other foot as it is commonly seen in both feet.
What treatment options are available for tarsal coalition?
Most cases of tarsal coalition find that the resultant injuries and symptoms heal with rest and avoiding strenuous weight-bearing activities and do not need surgical intervention however it is occasionally necessary to surgically intervene when the injuries and symptoms persist over a long period of time. Once it is discovered that a patient has an injury as the result of tarsal coalition they will have to initially have to rest and avoid aggravating activities. In most cases you may be initially required to avoid weight bearing and to use Crutches or a boot splint to reinforce and immobilize the foot. The doctor will most likely prescribe anti-inflammatory medication and painkillers for pain relief and to reduce any swelling. Patients will be referred through to a physiotherapist who will provide exercises to strengthen the ankle and foot muscles and ligaments to aid the healing process. It is vital that during the healing process the patient still tries to move a lot to reduce the risk of a DVT. Fluctuating pain levels will be experienced throughout the healing process however most of the discomfort towards the end of the healing process comes from stiffness levels caused by long term immobility. The rehabilitation exercises as well as massage and some manipulative therapies like Osteopathy or Chiropractic can aid in recovering your foot and ankle flexibility once the injury has healed.
It is very important that you see a podiatrist who can fully examine your feet and determine whether you need orthotics for your shoes. The podiatrist should also be able to provide you with advice on more appropriate and supportive training shoes. The failure to remedy these problems may result in a prolonged recovery or recurring injuries.