What are TMJ disorders?
TMJ disorders is the shortened term for painful conditions or problems related to the temporomandibular joint, the anatomical name for the jaw joint and its surrounding muscles. The TMJ joint is situated just in front of the ear connecting the temporal bone of the skull to the mandible bone that forms the jaw line. Like any joint, the TMJ is surrounded and supported by ligaments and muscles and has synovial fluid within its capsule to cushion any movement. However the TMJ is slightly different in that it has a small soft fibro cartilage disc, called the intra-articular meniscus, in between the two ends of the joint. This creates almost two separate compartments to the joint and is why the TMJ is so flexible. The upper half of the joint between the temporal bone and the soft meniscus is able to create the sliding movement forwards and backwards or side to side. The lower half of the joint, between the rounded end of the mandible called the mandibular condyle and the soft meniscus is responsible for the hinge movement of opening and closing the jaw. On opening the mouth, the condyle glides forward with the soft meniscus along the temporal bone socket and glides back when the mouth closes. The meniscus acts as a shock absorber for any impact, jaw grinding or chewing.
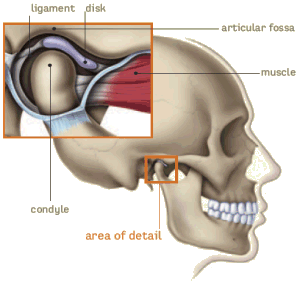
Three main categories of TMJ disorders
There are three main categories of TMJ conditions. The first category is myofascial pain which is the most common of all the TMJ disorders. The second is any injury to the inside of the joint complex such as a displaced meniscus, dislocated jaw or locked jaw. The third category involves rheumatoid arthritis or osteoarthritis affecting the TMJ. These categories are not exclusive as the joint and muscles work together meaning that often they may occur simultaneously to certain degrees.
What causes TMJ disorders?
The TMJ is a complex joint and disorders of the joint normally happen as the result of another behavior or condition. There are many theorized triggers for TMJ disorders however there is no conclusive research on these theories. The most commonly related factor is teeth clenching and grinding, medically referred to a “bruxism”. Patients may not be aware that they grind or clench their teeth but often it is pointed out to them by their partner who has heard them grind their teeth overnight or by their dentist who observes the wearing marks on the teeth. Bruxism is often the result of high levels of stress. Often in these cases people will wake up with painful aching jaw line muscles due to the over contraction of the main masseter muscle and in more severe cases, ear pain. It is thought that over time this activity can not only increase the wear on the teeth but also on the cartilage of the joint, possibly initiating future problems of osteoarthritis. Any habitual chewing of gum or biting of nails may also contribute to wear and tear of the joint and overuse of the muscle.
Any trauma that directly affects the jaw line, either dislocating it or even just gently overstretching it, has the potential to permanently injure the joint capsule, meniscus and ligaments. Dental problems such as a bite misalignment or tooth ache that causes you to favour one side of your mouth when eating, can cause or be the result of a TMJ problem. Rheumatoid arthritis generally only occurs in the TMJ when it has already been diagnosed somewhere else in the body.
It has been reported that in some cases of TMJ pain the pain was actually being referred from a neck condition and not being emitted by the actual TMJ joint itself.
What are the symptoms of a TMJ disorder?
The symptoms of a TMJ disorder most commonly start with a dull ache around the jaw which is often accompanied by a sharp pain on chewing movements. Often ear pain is noticed in front of and just below the ear, over the top of the joint line. This face pain has the ability to refer, resulting in 80 % of patients suffering from headaches. After trauma or with osteoarthritis, the jaw line can be extremely stiff and may lock when stretched too far or in certain directions. Jaw clicking happens to a large number of people and on its own is not indicative of a TMJ problem however painful clicking, popping, grinding or crunching sounds on jaw movement is common in TMJ disorders. In some cases additional symptoms such as dizziness and tinnitus are experienced.
How will a TMJ disorder be diagnosed?
There is no specific test for TMJ disorders; however your GP, therapist or dentist should be able to diagnose you through both listening to your symptoms and history and fully examining the jaw, face and neck. In most cases a full dental checkup will be advised, possibly with dental X-rays to rule out any tooth related pain. The dentist will also check your bite and jaw movement. If trauma is expected the further imaging of the TMJ and jaw line will be recommended. Due to the uncertainty of the cause of TMJ disorders, your GP or therapist will normally rule out any other conditions, such as infection, that may be responsible for the jaw pain, before making a conclusive diagnosis.
What treatments are available for TMJ disorders?
To begin with your GP may prescribe a short course of anti-inflammatory painkillers to reduce and control any painful inflammation. Due to the uncertainty of the root cause of TMJ disorders and a lack of definitive tests, conservative treatment options are normally advised. TMJ disorders are generally temporary and do not reach a chronic state, making conservative treatment normally highly effective. Surgery and more invasive treatment procedures, such as orthodontic surgery and TMJ replacement surgery, permanently alter the bite and joint and often make the condition worse.
Lifestyle changes are firstly advised, trying to deal with any stress levels that lead to bruxism is important, as is avoiding aggravating foods such as hard to eat toffees. Dental splints worn at night may help reduce the impact of any clenching or grinding, however the long term effectiveness of this is inconclusive. Try to avoid overstretching the joint during yawning or talking to prevent locking. Your GP or therapist will be able to advise you on when to start gentle stretches when these are done every day they are very affective in alleviating a stiff painful jaw. Applying a covered ice pack to the area may also significantly hasten the healing process by reducing the pain and swelling. Please make sure the ice pack is covered to prevent any ice burn and for best results use the icepack regularly for 10-15 minutes with intervals of 30 minutes.
Many people seek out alternative treatment to speed up the recovery process. Manipulative therapies such as chiropractic, osteopathy or physiotherapy may be helpful in stretching and mobilizing the TMJ. Acupuncture, massage therapy and therapies like Bowen technique are very good at alleviating and reducing any painful muscular tension or spasm.




.jpg)