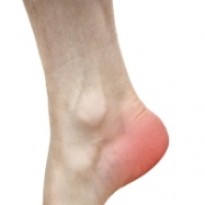
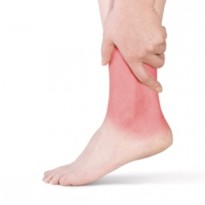
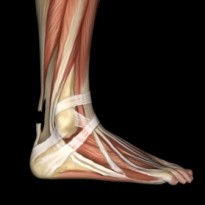
What is tibialis posterior tendonitis?
Tibialis anterior tendonitis, also known as tibialis anterior tendinopathy, is the medical term for tissue damage to and inflammation of the tibialis posterior tendon. The tendons in the body connect the muscles to the bones, their structure is very similar to a rubbery stretchy cord making it strong, durable and flexible. Where the tendons attach to the bone they are covered in a sheath that is lubricated on the inside, allowing the tendon to move in and out effortlessly. Joint movement is the end result of the muscle fibres contracting and pulling on the tendon which in turn tugs at the bone producing the movement. The tissue damage and inflammation that cause tendonitis occur around the tendon itself, any damage to the tendon sheath is termed tenosynovitis, although it is very common for both conditions to be present at the same time. Tendonitis makes any movement of that tendon very painful and stiff.
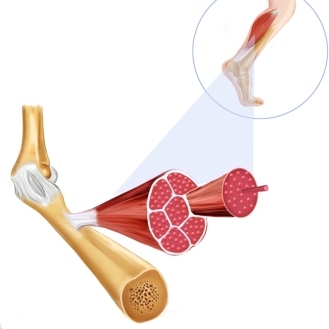
Why & when does tibialis posterior tendonitis happen?
Tibialis posterior tendonitis is a common injury and effects people of all ages. It is normally seen in individuals who partake in athletic sports that involve repetitive or forceful inversion and plantar flexion of the ankle and foot. The tibialis posterior muscle is situated along the inside of the lower leg originating just behind the knee, running down the inside of the leg, into the foot and attaching onto several of the bones in the middle of the foot via the tibialis posterior tendon. The tibialis posterior muscle is responsible for inversion (tilting the ankle and foot so that the sole of the foot points inwards) and plantar flexion (pointing the toes downwards) of the foot and ankle. Overuse of this tendon through repetitive, high force and traumatic dorsiflexion of the foot and ankle will lead to tibialis posterior tendonitis. Typically activities such as running and walking on uneven surfaces can trigger the onset.
What does tibialis posterior tendonitis feel like?
Tibialis posterior tendonitis begins as a dull ache around the inside of the ankle that gradually worsens over a course of 2-3 weeks. In some cases the discomfort is only felt on ankle inversion or plantar flexion when the tibialis posterior tendon is stressed and with others, it is felt once resting after an activity that involves ankle inversion and plantar flexion. Stiffness and dull aches are normally experienced during the night and are most intense early in the mornings. The pain and discomfort is not always restricted to the front of the ankle and often radiates up into the inside of the lower leg or down into the top of the foot. The inside of the ankle and top of the foot will be tender to touch and on occasion there may be minor swelling around the area.
How long does tibialis posterior tendonitis take to heal?
Mild cases of Tibialis posterior tendonitis can recover in as little as 3 days to 2 weeks with treatment, whereas moderate or chronic cases of tendonitis take much longer. However as long as the aggravating ankle inversion and plantar flexion has been avoided during recovery then most cases of tibialis anterior tendonitis will have fully healed within 6 weeks. If you experience pain longer than 6 weeks it is advisable to attend your GP.
How will tibialis posterior tendonitis be diagnosed?
Your GP or therapist will be able to diagnose you by both listening to your history and examining you. No X-rays or further investigation should be needed to confirm diagnosis.
What treatment options are available for tibialis posterior tendonitis?
Your GP will most likely prescribe anti-inflammatory medication and painkillers for pain relief and to reduce any swelling. You will be advised to follow the R.I.C.E protocol. The R.I.C.E protocol involves Resting your ankle, try not to walk about on it too much and most importantly avoid all ankle eversion movements. Ice, applying a covered ice pack to the area may also significantly hasten the healing process by reducing the pain and swelling. Make sure the ice pack is covered to prevent any ice burn and for best results use the icepack regularly for 10-15 minutes with intervals of 30 minutes. Compression, try and keep the elastic bandage on during the day to limit the swelling and be sure to take it off at night. Elevation, keep your foot raised on cushions or a stool to help limit the swelling.
Your GP or therapist will be able to provide you with exercises to strengthen the ankle ligaments and stretch the tibialis posterior muscle to aid the healing process and prevent reoccurring injury. Many people find massage therapy helpful to loosen the affected tibialis posterior muscle, manipulative therapies such as physiotherapy, chiropractic and osteopathy are thought to help through mobilisation treatment of the ankle, working to reduce any stiffness levels and return the joint back to its normal movement.
If your GP has mentioned or if in-fact you feel that there is some element of foot or ankle dysfunction that has predisposed you to this injury then it is very important that you see a podiatrist who can fully examine your feet and determine whether you need orthotics for your shoes. Often inappropriate and unsupportive running shoes are a factor in the development of ankle or foot tendinitis. The failure to do this may result in recurring cases of tendonitis.