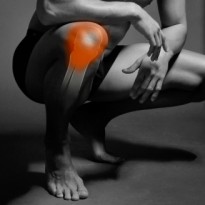
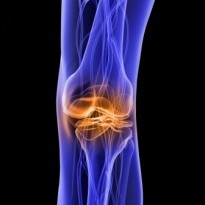
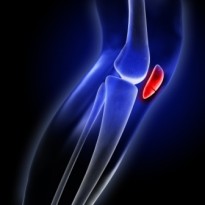
What is pre-patellar bursitis?
Pre-patellar bursitis, also known as housemaid’s knee, is the painful inflammation and swelling of the pre-patellar bursa that is situated between the skin and the knee cap. A bursa is a small fluid filled sac that forms around joints in areas where there is a lot of friction between muscles, tendons and outcrops of bone. The bursae position themselves in between the tendon or muscle and the bone, buffering any friction from movement. To picture a bursa imagine it as a very small water filled balloon that sits in places where things rub against each other, such as in between a tendon and a bone to provide a soft smooth cushion for the tendon to pass over painlessly. The covering of the bursa also acts as a lubricant and helps the tendons movement. It is estimated that there is over 150 bursae in your body all with the job of protecting the joint and tendons from wear and all are very small and unnoticeable until they become swollen and painful with bursitis.
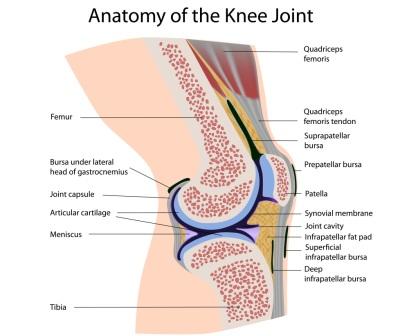
Why & when does pre-patellar bursitis happen?
Pre-patellar bursitis can be caused through injury, infection or can be triggered by certain health conditions. If bursitis develops as a result of injury then it will normally be due to continuous pressure, such as kneeling or repetitive strenuous activity. These factors put more pressure over the bursa, irritating it and triggering a painful inflammatory reaction (swelling). This risk of developing bursitis in this way is greater in those whose jobs or hobbies involve a lot of repetitive movements, for example carpet fitters and gardeners who spend a lot of time kneeling and so are more at risk of bursitis in the knee. Runners have a greater likelihood of developing bursitis in the hip. Bursitis can also be brought on by excessive pressure or direct impact trauma, for example banging your elbow or dropping on to your knees. Infection is a less common cause of bursitis and normally only occurs in people who have a weakened immune system from other health issues. The infection can work its way to the bursa from a cut close to the bursa that has become infected, in these cases the bursitis is termed as septic bursitis. Certain health conditions can also trigger the development of bursitis such as rheumatoid arthritis and gout, amongst others.
Pre-patellar bursitis is very similar to infra-patellar bursitis as the bursae are very close in proximity and symptoms are almost identical, however pre-patellar bursitis is a lot more common.
What does pre-patellar bursitis feel like?
The symptoms of bursitis vary depending on whether it is the result of injury or an underlying health condition or from infection. In cases of normal overuse and injury the pain is normally a constant dull ache or burning pain around the knee cap that is aggravated by any touch, pressure or movement of the knee joint. There will normally be notable swelling around the knee. In other cases where the bursa lies deep under the skin, such as in the hip or shoulder swelling might not be visible. Movement of the knee will be stiff, especially in the mornings and after any activity involving the joint. All of these symptoms are experienced with septic bursitis with the addition of a high temperature of 38ºC or over and feverish chills. The skin around the affected joint will also appear to be red and will feel incredibly warm to the touch.
In cases of septic bursitis it is important that you seek medical attention. With injury induced bursitis if symptoms still persist after 2 weeks then report to your GP.
How long does pre-patellar bursitis take to heal?
The healing time frame of pre-patellar bursitis can vary from 2 to 8 weeks and in some cases even longer than that. Depending on the severity of the injury or the location. If the bursitis occurss near a joint that can be rested easily the healing time will be greatly reduced. On the other hand, if it is in a joint that is regularly used, such as the knee, then this perpetuates and flares the condition making healing more of a lengthy process.
How will pre-patellar bursitis be diagnosed?
Your GP or therapist will be able to diagnose you by both listening to your history and examining you. No X-rays or further investigation should be needed to confirm diagnosis but may be requested to check for any underlying health conditions that may have triggered the bursitis.
What treatment options are available for pre-patellar bursitis?
Your GP may prescribe a short course of anti-inflammatory painkillers to reduce and control the painful inflammation that occurs and antibiotics in cases of septic bursitis. Applying a covered ice pack to the area after the initial injury may also significantly hasten the healing process by reducing the pain and swelling. Please make sure the ice pack is covered to prevent any ice burn and for best results use the icepack regularly for 10-15 minutes with intervals of 30 minutes. Where possible it is advisable to avoid all aggravating movements and postures, however complete rest is not advised as this can lead to weakness and further shortening of the muscle. Massage and manipulative therapies can help loosen the surrounding muscles and tendons of the affected joint, reducing the pressure over the bursa and allowing faster healing. If the bursitis is chronic and not responding to treatment then your GP may refer you for a corticosteroid injection which will reduce the inflammation levels which will in-turn reduce the pain levels experienced. Corticosteroid injections can have varied results. Surgery is a rare option when it comes to bursitis but occasionally it may be necessary in extremely chronic cases or to drain an infected bursa.
The underlying cause of the bursitis must be identified to prevent further reoccurrences. Failure to eliminate the cause will lead to future flare ups and a poor and slow recovery. Future occurrences can be prevented with the use of stretches and strengthening exercises which will help prevent your muscles from tightening up over the bursa, Pilates and yoga are very good for this providing the aggravating movements are avoided. Wearing joint supports such as knee pads or elbow supports may also reduce your likelihood of redeveloping bursitis.