What is rheumatoid arthritis of the elbow?
Rheumatoid arthritis (RA) is an autoimmune disease. The immune system normally fights off infections and strange germ cells in the body keeping you well and healthy from day to day. In cases of rheumatoid arthritis the immune system mistakes cells that line your joints for foreign unknown cells which pose a threat to your body. Once your immune system attacks the joint line cells your joint will swell up and stiffen with the high inflammation levels. Over time, this can damage the joint itself, the cartilage and nearby bone.
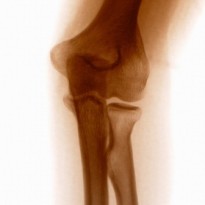
The Elbow joint itself is formed by the union of the far end of the humerus (the upper arm bone) and the radius and ulna (the forearm bones). The end of the ulna is called the olecranon process this hooks into the back of the humerus creating what is known as a hinge joint, named as such as it only moves in flexion and extension. It is the joints between the radius and ulna that allow you to pivot your hand and forearm from palm upwards to palm downwards actions, known as supination and pronation.
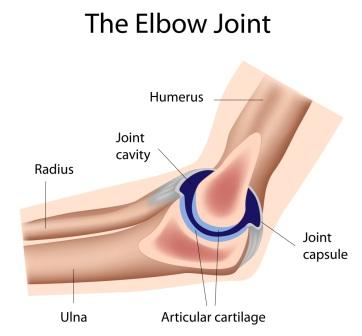
The boney surface of each joint is known as subchondral bone. Either side of the joints subchondral bone never meet as they are separated by a protective layer of articular cartilage which covers both boney surfaces. In addition, there is small amount of thick fluid called synovial fluid that cushions the joint ends. This is then encased in a strong connective tissue capsule that contains the entire elbow joint. The smooth cartilage, fluid and capsule allow each joint to move in a smooth, flexible and stable manner. When the cells decide to attack they target the synovium cells on the inside of the capsule, this process creates large amounts of inflammation causing the joint to swell quite dramatically. The severe painful swelling not only creates an extremely stiff joint but over time with recurrent attacks, chemicals released by the high levels of inflammation can thicken the synovium damaging the articular cartilage and even the subchondral bone of the joint. This will worsen symptoms and leave joints painful and stiff between flare ups. The surrounding tendons and ligaments are also affected by these attacks, causing them to weaken. This causes the joint to become lax with no support, allowing it to shift and loose its original shape and alignment.
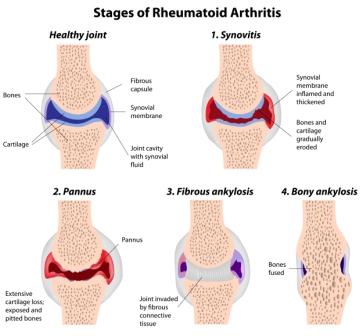
Why & when does rheumatoid arthritis happen in the elbow?
Rheumatoid arthritis is just one of many types of arthritis affecting the joints of the body. Osteoarthritis is the most common type of arthritis in the UK, but rheumatoid arthritis is quite common affecting one in every 100 people with an estimated 400,000 people living with the condition in England and Wales alone. The condition affects three times as many women as men and normally develops between the ages of 40 to 50, although it can affect people at any age.
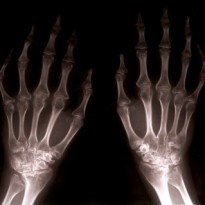
RA has the ability to develop in any joint of the body but most commonly it affects the feet, ankles, wrists and hands. Elbow RA is slightly less common as is RA affecting the Hip, knees and spine. One characteristic of RA is that it normally develops symmetrically affecting the same joint on both sides of the body.
There is a lot understood about how RA attacks the joint and manifests, however there is still no understanding of what triggers the autoimmune disease to develop in the first place. There have been relatable links to certain viruses, infections and hormones, and even genetically linked through familial history. Scientific research for these links has so far been inconclusive.
Patients with RA also tend to be more likely to develop other conditions such as osteoporosis, cardiovascular disease, carpal tunnel syndrome, tendon ruptures, high blood pressure levels and inflammation of other parts of your body like the lungs, heart, eyes and even blood vessels.
What does rheumatoid arthritis in the elbow feel like?
In cases of elbow rheumatoid arthritis the sufferer will most likely have already experienced symptoms or may be diagnosed with RA in the small joints of the hand or foot. Symptoms normally develop gradually over several weeks or in some cases months. Occasionally there are cases of sudden onset RA that develop over a few days. These cases might be quick in onset and recovery and several episodes like this may happen before symptoms become more constant. In some cases symptoms like muscle pain, fever, weight loss and anaemia precede the joint pain and symptoms.
The first symptom you experience may be joint and muscle stiffness, particularly in the early mornings with symptoms starting to ease a few hours after getting up. This presentation is very similar to osteoarthritis which also develops stiffness which is worse in the mornings the main distinction at this point between the two conditions is that OA joint stiffness loosens after half an hour of moving whereas RA takes much longer, up to a couple hours.
After a few weeks the same joints that have been stiff may become painful and swollen. The pain will feel like a deep, throbbing ache that is aggravated by rest and certain levels of activity. The pain levels can be quite severe during a flare up causing incredible discomfort for patients, in particular those with multiple joints affected. The swelling levels during a flare up also cause the skin around the joint to be extremely tender and slightly warm to the touch. The severity and frequency of episodes or flare ups will vary greatly between patients, although they will normally attack and be at their greatest in the mornings.
How will rheumatoid arthritis in the elbow be diagnosed?
Your GP will be able to make a preliminary diagnosis by both listening to your symptom history and carefully examining the affected joints.
Further testing is normally needed to confirm the preliminary diagnosis. To do this your GP will refer you to a Rheumatologist (a specialist who deals with rheumatic diseases). Your GP may also want to do a blood test to look for certain factors such as ESR and rheumatoid factor amongst others that are normally found in RA patients. This however is not a conclusive test but merely a strong indication of the conditions presence. An X-ray of the affected area is normally recommended to confirm the diagnosis occasionally and MRI may be used to further evaluate the level and extent of the joint damage. Some GPs will use in clinic musculoskeletal ultrasound to identify the presence of the condition in a joint, however this is not always an available option.
The referral time to your Rheumatologist is normally well within three months. The earlier a diagnosis can be made and treatment started the better as any damage done to the joint is permanent.
What treatment options are available for rheumatoid arthritis?
Unfortunately there is no cure for rheumatoid arthritis. Instead treatment is normally aimed at reducing pain and inflammation levels and preventing further damage to the joints. Your GP and Rheumatologist will be able to prescribe you medication such as disease-modifying antirheumatic drugs (DMARDs) or non-steroidal anti-inflammatory drugs (NSAIDs)that will help control the condition and alleviate some of the daily symptoms.
Sufferers normally opt for a combination of drug and conservative treatments, most importantly modifying their lifestyle and avoiding or adapting certain activities to minimise any potential discomfort but still allowing them to remain as active as possible. It is incredibly important for people who are overweight to factor in weight loss as part of their treatment as it has been shown to help reduce pain and stiffness levels in particular cases where the knees and hips are involved. If this is a concern then it is advisable to consult a dietician or nutritionist who can examine your daily diet and suggest where and what improvements you could make. Rest is important through the severe flare ups but it is equally important to start lightly exercising as soon as you feel you can. Light exercises provided by your therapist or trainer will not only strengthen your joint but also maintain its flexibility and help prevent any further stiffness. Many sufferers find mild manual manipulative therapies like chiropractic, osteopathy and physiotherapy to be helpful in preventing general day to day stiffness and pain levels and in keeping joints mobile. Manipulative therapies are not advised during a flare up. Massage therapies and Bowen technique have also been found to help loosen the muscle spasm around the joint.